U.S. Army veteran George “Mike” Egan served as a 1st Air Cavalry helicopter door gunner and crew chief during the Vietnam War. He suffered a lower back injury and shrapnel-riddled legs when his helicopter was shot down. He spent a week in a field hospital, finished his tour, and was honorably discharged with a Purple Heart.
Mr. Egan eventually settled down near Columbia, SC and worked as a contractor. His back pain became unbearable and forced him to seek treatment at the local VA hospital. An MRI at the VA showed a massive disc extrusion that severely compressed the cauda equina nerves in his lower spine.
Mr. Egan needed a spine surgeon to treat the problem by surgically decompressing the nerves. Otherwise, he would inevitably develop permanent nerve damage called cauda equina syndrome and lose function and sensation below the waist. Instead, Mr. Egan’s VA providers gave him drugs to manage his pain for more than 18 months and refused to refer him to a spine surgeon until after he suffered incontinence and lost the ability to walk.
Mr. Egan permanently lost control of his bowels and bladder, and he requires assistive devices to stand. Attorneys Jim Matthews and Lee Atkinson filed a lawsuit against the United States, proved that the VA’s care was grossly negligent, and secured a $3,225,000 settlement for him on the eve of trial.
See what Mr. Egan had to say on Google about our firm’s representation:
An Obvious Diagnosis Followed by a Long Battle for Adequate Care
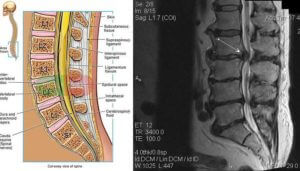
The lumbar spine is in the lower back and is divided into five numbered vertebral disc spaces: L1, L2, L3, L4, and L5. L1 is at the top, or closest to the head, and L5 is at the bottom, or closest to the feet. Below L1, the spinal cord tapers into the cauda equina nerves, which are a bundle of individual nerves that resemble a horse’s tail. The cauda equina nerves are an extension of the spinal cord. The individual nerves go to and innervate (provide motor and sensor function) different parts of the lower body. When the nerves are permanently injured, the body parts that they innervate lose sensation and function.
Mr. Egan’s VA medical providers initially attempted to treat his back pain conservatively with drugs and physical therapy. His pain did not respond to the conservative treatments and he underwent an MRI of his lumbar spine on October 25, 2010. The MRI showed that a ruptured disc obliterated 95 percent of the spinal canal around the cauda equina nerves at L2-3. The practical effect was that the nerves were placed under severe pressure. Over time, the nerves would suffer permanent injury unless they were decompressed.
The VA hospital had a neurosurgery department, but did not have any neurosurgeons and staffed the department with a nurse practitioner who worked under the supervision of a general surgeon. Rather than send Mr. Egan to another hospital with a spine surgeon, his VA providers kept him in-house and persisted in attempting to relieve his pain with injections and oral drugs that did nothing to relieve the pressure on the cauda equina nerves. When Mr. Egan reached the point that it was unsafe for him to have any more injections for several months, his VA providers planned to send him to an in-house behavior therapist rather than a spine surgeon at another facility.
After almost sixteen months of ineffective treatment, Mr. Egan woke up in excruciating pain and was unable to stand. He was admitted to the VA hospital in Columbia on February 21, 2012, and underwent another MRI that showed his nerves were still severely compressed. His VA providers heavily drugged him and planned to send him home, but his wife begged them to let him stay one more night. Over the course of that night, the drugs caused Mr. Egan to develop severe delirium. He was put in a medically induced coma for weeks. When he finally came to, he realized that he lost sensation and function in his legs and couldn’t control his bowels and bladder. Despite the obvious cause of his symptoms, his VA providers refused to send him to a spine surgeon until April 11, 2012. He underwent decompression surgery on April 12, but several of his cauda equina nerves were already permanently injured by that point.
Mr. Egan Suffers Permanent, Life Changing Injuries
The result of the VA providers’ failure to simply send Mr. Egan to a spine surgeon sooner is that he has permanently lost the ability to sense when he has to urinate or have a bowel movement, he has lost sensation in his legs below his knees, and he has a condition called foot drop in both feet because he has lost the ability to raise them. He can walk short distances with the aid of a rolling walker and braces on his feet, but primarily relies on a wheelchair to move around.
Mr. Egan’s Recovery of Monetary Damages Was Limited Unless He Could Prove Gross Negligence
While any medical malpractice case is challenging, this one was especially so. Because of tort reform in South Carolina, compensation for pain and suffering in medical malpractice cases is currently limited at about $450,000 unless the injured person proves the hospital and doctors were grossly negligent. While negligence is the failure to exercise ordinary care, gross negligence is the failure to exercise even slight care or demonstrating inadvertence to the point of recklessness.
Holding the VA Responsible
Jim Matthews and Lee Atkinson were determined to hold the VA accountable and maximize the Egan’s recovery by proving gross negligence. They hired nationally recognized medical specialists to serve as expert witnesses and established through numerous depositions that the various VA providers inexcusably neglected Mr. Egan’s obvious nerve compression. Importantly, they convinced the court to preclude the United States from using any of its own expert witnesses. As the trial neared, the United States was forced to acknowledge the likelihood that the VA providers would be found grossly negligent and settle the Egan’s claims.
While no amount of money can make up for the loss Mr. Egan suffered, we are proud to represent him and his wife, and help them secure compensation that will provide for the medical care he needs and help them have the quality of life they deserve.