Dehydration in Georgia Nursing Homes
Nursing homes and other long-term care facilities are responsible for ensuring residents are accurately hydrated.
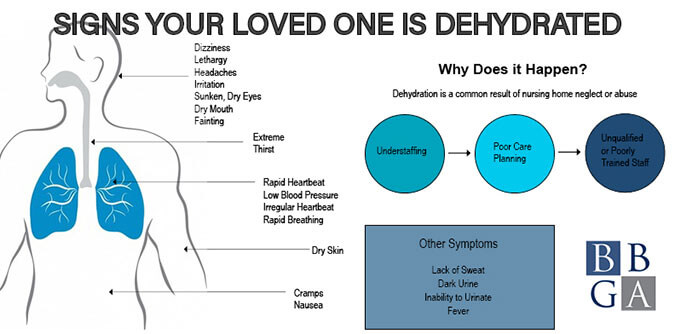
Unfortunately, due to understaffing, improper care planning, disorganization, and unqualified or poorly trained staff, many elderly or disabled residents in Georgia nursing homes don’t receive the proper amount of fluids to stay adequately hydrated.
IF YOU SUSPECT NURSING HOME ABUSE OR NEGLECT DUE TO DEHYDRATION, CONTACT US ONLINE OR CALL (706) 354-4000 TODAY. WE HOLD GEORGIA NURSING HOMES ACCOUNTABLE.
Symptoms of Dehydration: How to Know if Your Loved One is Dehydrated
If your loved one experiences any of the following symptoms, it could be a result of dehydration:
- Extreme or chronic thirst
- Dry mouth/lips
- Dry eyes
- Sunken eyes
- Dizziness
- Lethargy
- Headaches
- Irritation/emotional outbursts
- Fainting
- Rapid or erratic heartbeat
- Low blood pressure
- Rapid or shallow breathing
- Dry skin
- Stomach cramps
- Nausea
- Inability to sweat
- Dark urine
- Kidney failure
- Inability to urinate or infrequent urination
- Fever
- Urinary tract infection
- Constipation
- Pressure injuries
- Unconsciousness
Dehydration is also a common result of nursing home abuse or neglect and can lead to more serious complications, and ultimately, comatose or death. When long-term care facilities are chronically understaffed, fail to adequately train their employees, or if nursing home staff don’t understand a resident’s needs for fluids, this is considered neglect.
Many nursing home residents are unable to express their needs for various reasons. Some are unable to swallow or speak, others may have Alzheimer’s or dementia and aren’t aware how long it’s been since they’ve eaten or taken in fluids. It’s the nursing home’s responsibility to ensure every resident is properly cared for, and that includes diet and fluid intake.
What Happens When Someone is Dehydrated?
As we age, the body naturally loses water, so it’s important to increase our intake of water to stay healthy and hydrated. Because water is an essential sustenance, when we fail to hydrate our bodies, they begin to shut down.
It may start with a minor headache, extreme thirst, and lethargy, but the longer a body goes without proper fluids, the faster the body and its organs begin to decline.
Here are a few examples of what happens when someone is dehydrated:
- According to the U.S. National Library of Medicine, even mild dehydration negatively affects mood, attention, memory and motor skills. This may be due to brain tissue fluid decrease
- Kidneys retain more water to overcompensate, making urination less frequent
- Without proper hydration, it’s more difficult for the body to regulate temperature, which can cause hypothermia
- As a person becomes more dehydrated, their blood becomes more concentrated, so it’s more difficult for the heart to maintain a healthy blood pressure
- The risk of exhaustion or collapse increases due to low blood pressure
- In severe cases, blood pressure and blood volume can drop so low that the body goes into hypovolemic shock, which is a life-threatening condition that occurs when you lose more than 20 percent of your body’s blood or fluid supply
- When the heart is unable to pump enough blood, organs begin to shut down
Combating Dehydration in Nursing Homes: What Caregivers Should be Doing
Nursing homes and other long-term care facilities are responsible for the well-being of its residents. Caregivers and other staff can successfully combat dehydration with the proper steps and protocols in place.
Here are a few things caregivers should be doing to ensure your loved one is receiving adequate fluids each day:
- Properly training staff
- Implementing Resident Assessment Protocol/MDS Assessment. The Minimum Data Set (MDS) is a U.S. federally mandated process for clinical assessment of all residents in Medicare or Medicaid certified nursing homes
- Ensuring residents always have water within their reach
- Monitoring residents’ fluid intake daily
- Encouraging moderate, frequent drinking
- If a resident isn’t consuming the proper amount of fluid for their body weight, staff should be increasing their amount of fluid intake gradually
- Monitoring residents’ urination frequency (color of urine should be light, clear, or pale yellow)
- Minimizing residents’ alcohol and caffeine ingestion
- Replenishing electrolytes with a sports drink such as Gatorade
- Incorporating foods high in water such as fresh fruits and vegetables
- Severe dehydration requires prompt medical attention. If a resident is severely dehydrated, caregivers and nursing home staff should contact the resident’s doctor at the first signs of dehydration
Is Dehydration a Symptom of a Bigger Problem?
The simple answer is, yes! A nursing home resident should never have to suffer from dehydration. Proper attention and care includes keeping residents healthy and hydrated.
Contact an Experienced Georgia Nursing Home Abuse Lawyer
If your loved one is showing signs of dehydration and they live in a nursing home or long-term care facility, contact us online or call (706) 354-4000 today for a free consultation.
