
In nearly every labor and delivery room, there is a steady rhythmic sound that becomes part of childbirth. The fetal heart monitor records the baby’s heartbeat and the mother’s contractions in real time. For many parents, that sound is reassuring. For medical professionals, the tracing on the monitor is one of the most important clinical tools available during labor.
When properly interpreted and acted upon, fetal heart monitoring can help prevent catastrophic injury. When misread, ignored, or improperly managed, the consequences can be permanent.
In this fourth installment of our Childbirth Injury Series, we look more closely at fetal heart monitoring strips, how they are used, how they can fail, and why they often become central to understanding what happened during a complicated delivery.
What Is Fetal Heart Monitoring?
Fetal heart monitoring, also called cardiotocography (CTG), Electronic Fetal Monitoring (EFM), or fetal heart rate monitoring, tracks two things during labor: the baby’s heart rate and the mother’s uterine contractions. The information appears as a continuous tracing, commonly referred to as a strip.
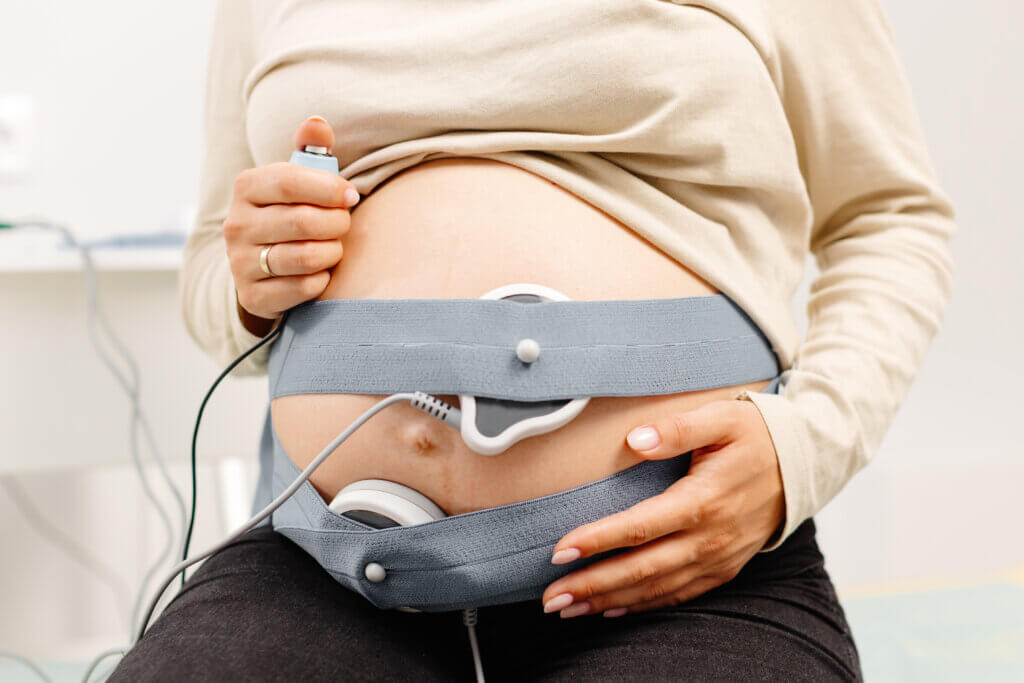
Monitoring may be external, using belts placed around the mother’s abdomen, or internal, using a fetal scalp electrode attached to the baby and a pressure catheter placed in the uterus to measure contractions more precisely.
The tracing shows the baby’s baseline heart rate, beat to beat variability, accelerations, decelerations, and the timing and strength of contractions. Together, this information helps the medical team determine whether the baby is tolerating labor safely.
Although fetal monitoring is most often associated with detecting oxygen deprivation, it reflects more broadly how the baby responds to stress. That stress may result from reduced oxygen delivery, but it can also be caused by umbilical cord compression, excessive contractions from medications such as Pitocin, maternal infection, placental problems, or sudden complications like uterine rupture. The monitor does not diagnose these conditions directly. It shows how the baby is responding in real time, allowing providers to investigate the cause and intervene when necessary.
Because contractions temporarily reduce blood flow to the placenta, a baby must tolerate repeated decreases in oxygen. Most healthy babies can. But when oxygen deprivation becomes prolonged, or when other complications place sustained stress on the baby, the risk of serious injury can rise quickly.
How Strips Are Interpreted
Obstetrics uses a three-tier system to classify fetal heart rate tracings as normal, indeterminate, or abnormal.
A normal tracing generally reflects a reassuring baseline heart rate with moderate variability and no concerning decelerations. An indeterminate tracing requires close observation and sound clinical judgment. An abnormal tracing may show absent variability, recurrent decelerations, or significant slowing of the heart rate, all of which can signal that the baby is not tolerating labor safely.
While these categories provide structure, interpretation is not purely mechanical. It requires training and experience. Two providers may sometimes view the same strip differently. That subjectivity can become critically important when questions arise about whether earlier intervention was necessary and appropriate.
How Fetal Monitoring Can Go Wrong
One of the most significant vulnerabilities in fetal monitoring is human interpretation. Subtle changes can signal a developing problem long before a crisis occurs. A gradual loss of heart rate variability, recurrent late decelerations, or a prolonged deceleration lasting several minutes may reflect worsening oxygen deprivation or another serious issue. If those warning signs are overlooked, the opportunity for safe intervention can narrow quickly.
Delayed response is another common concern. Recognizing distress is only the first step. The more important question is how quickly the medical team acts. When a strip shows persistent signs that a baby is not tolerating labor, a timely cesarean section may be necessary. Delays in decision making, communication, or operating room access can have serious consequences when a baby is under sustained stress.
Technical limitations also exist. External monitors can shift, lose signal, or mistakenly record the mother’s heart rate instead of the baby’s. In some cases, an internal monitor would provide clearer data, but it is not placed promptly. Poor signal quality can create false reassurance or make it harder to recognize when the baby’s condition is worsening.
Labor inducing medications add another layer of risk. Drugs such as Pitocin are used to strengthen contractions, but contractions that occur too frequently can reduce oxygen delivery and increase fetal stress. Careful monitoring and appropriate adjustment of medication are essential.
What Training Do Providers Receive?
Labor and delivery nurses receive specialized education in fetal heart rate interpretation, and many hospitals require certification courses and ongoing competency assessments. Obstetricians receive training during residency and are expected to maintain proficiency throughout practice.
Even so, training standards, hospital protocols, and real-world application can vary. When a child suffers a serious injury, reviewing staff training and adherence to accepted standards of care is often necessary to understand whether preventable mistakes occurred.
What Happens When Intervention Is Delayed?
When oxygen deprivation or severe stress continues without timely intervention, the consequences can be devastating.
For the baby, prolonged oxygen deprivation, known medically as hypoxia, can lead to serious injury. One of the most severe outcomes is hypoxic ischemic encephalopathy, often called HIE, a type of brain injury caused by a lack of oxygen and blood flow to the brain. HIE can result in conditions such as cerebral palsy, seizure disorders, developmental delays, and permanent motor impairment. Some children require lifelong medical care and support. In the most tragic cases, the outcome can be fatal.
For the mother, delayed intervention can increase the risk of emergency surgery, hemorrhage, infection, and lasting emotional trauma. A complicated delivery may also affect future pregnancies.
These are life altering injuries that impact families for decades.
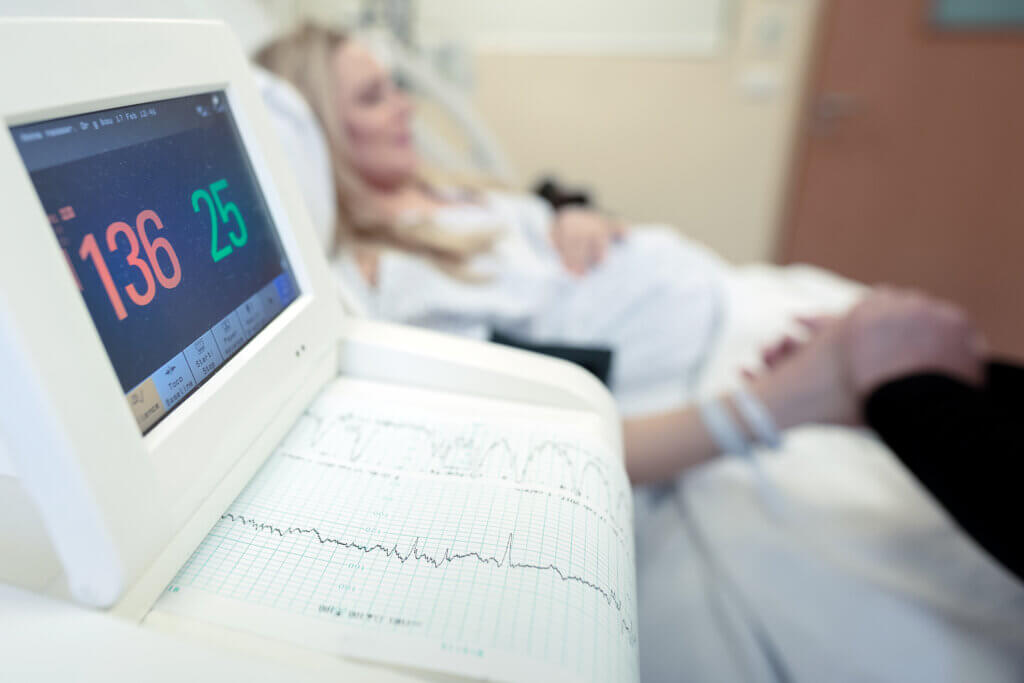
Preservation of Fetal Monitoring Strips
Fetal monitoring strips, also known as tracings, are part of the medical record. In modern hospitals, they are usually stored electronically within the medical record system. In some facilities, paper strips are scanned and archived after delivery.
Hospitals maintain retention policies that determine how long these records are preserved, often for many years. When a serious birth injury is suspected, the fetal monitoring strip frequently becomes critical evidence.
Questions sometimes arise about missing segments of tracings, gaps in documentation, or entries made after the fact. Electronic systems typically contain audit trails that track when records are created or modified. A complete and careful review of the record, including electronic metadata, is essential when evaluating what occurred during labor. Our attorneys work with qualified medical and technical experts to ensure that these records are thoroughly examined.
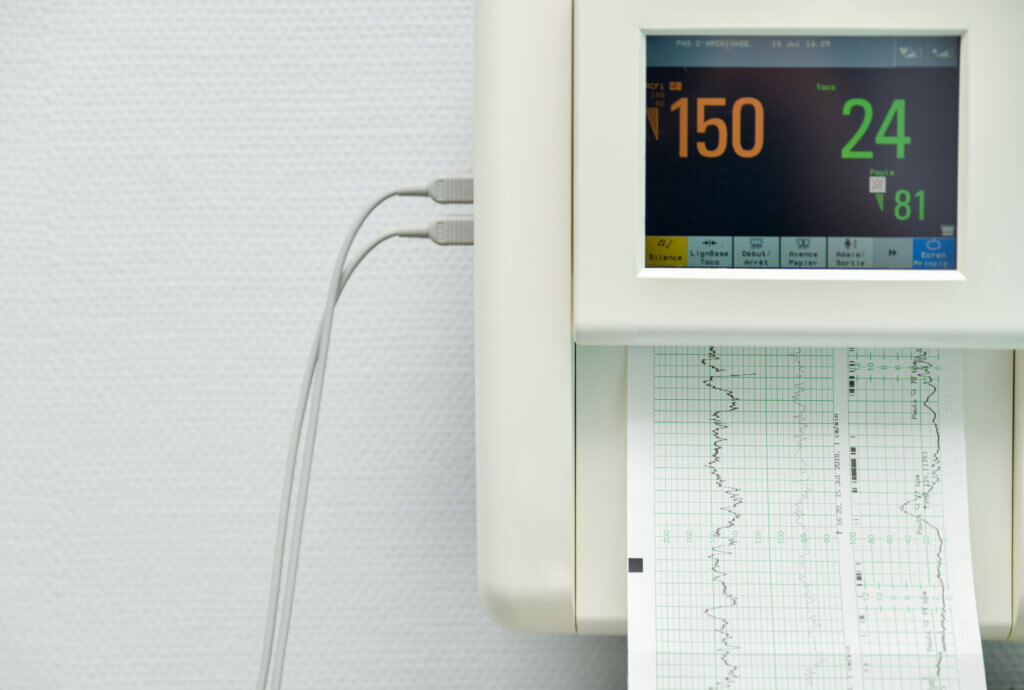
How Fetal Monitoring Helps Explain What Happened
In many complicated birth cases, the fetal heart monitoring strip provides a detailed timeline of events. Medical experts can analyze the tracing minute by minute and compare it with medication records, physician involvement, and the timing of delivery.
The strip may show when signs of distress first appeared, whether they worsened, and whether appropriate interventions were attempted. It can also be evaluated alongside laboratory results and the baby’s condition at birth to help determine whether injury occurred during labor.
Because these cases involve complex medical issues, careful review of fetal monitoring data is often one of the most important steps in understanding whether a birth injury may have been preventable.
Why This Matters for Families
Families are often told that a difficult delivery was unavoidable. They may be reassured that the monitor looked fine or that nothing could have been done differently.
Fetal monitoring exists to detect warning signs before permanent harm occurs. When properly used, it can prompt timely intervention and protect a child’s future. When warning signs are missed or ignored, the consequences can last a lifetime.
At Blasingame, Burch, Garrard and Ashley, our birth injury team works closely with qualified medical experts to conduct detailed reviews of labor and delivery records, including fetal monitoring strips. If your child suffered a serious injury during labor or delivery and you have questions about whether warning signs were missed, our team can help you better understand your legal options.
Related Articles in our Childbirth Injury Series
Leaders in Birth Injury Litigation: BBGA Attorneys Evan Jones and Lee Atkinson
Cerebral Palsy and Birth Injuries: What Parents Should Know
Erb’s Palsy and Brachial Plexus Injuries: What Parents Should Know

